Sickle cell anaemia (SCA) is reported to be the 12th leading cause of death worldwide in children below the age of 5 years*.
As per recent news reports, sickle cell anaemia is becoming one of the major public health concerns in India. It is estimated that India has the second-highest burden of this disease, with over 2 crore people with sickle cell traits and 14 lakh people with sickle cell disease.
Because of increasing severity and spread of this disease, the health ministry has released the standard treatment guidelines for Sickle Cell Anaemia Disease in May this year and hass urged people to follow the same.
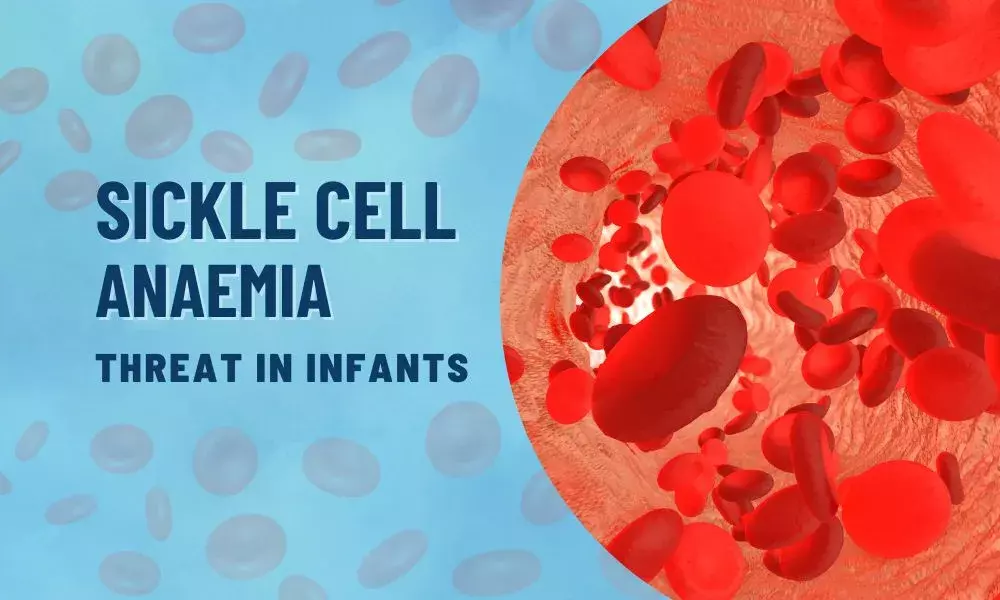
Sickle cell anaemia or sickle cell disease is a genetic disorder, it affects the shape of red blood cells, which carry oxygen to all parts of the body.
Red blood cells are usually round and flexible, so they can move easily through blood vessels. In sickle cell anaemia, some red blood cells are shaped like sickles or crescent moons. These sickle cells become rigid and sticky, which can slow or block blood flow. These cells generally form during fetal development.
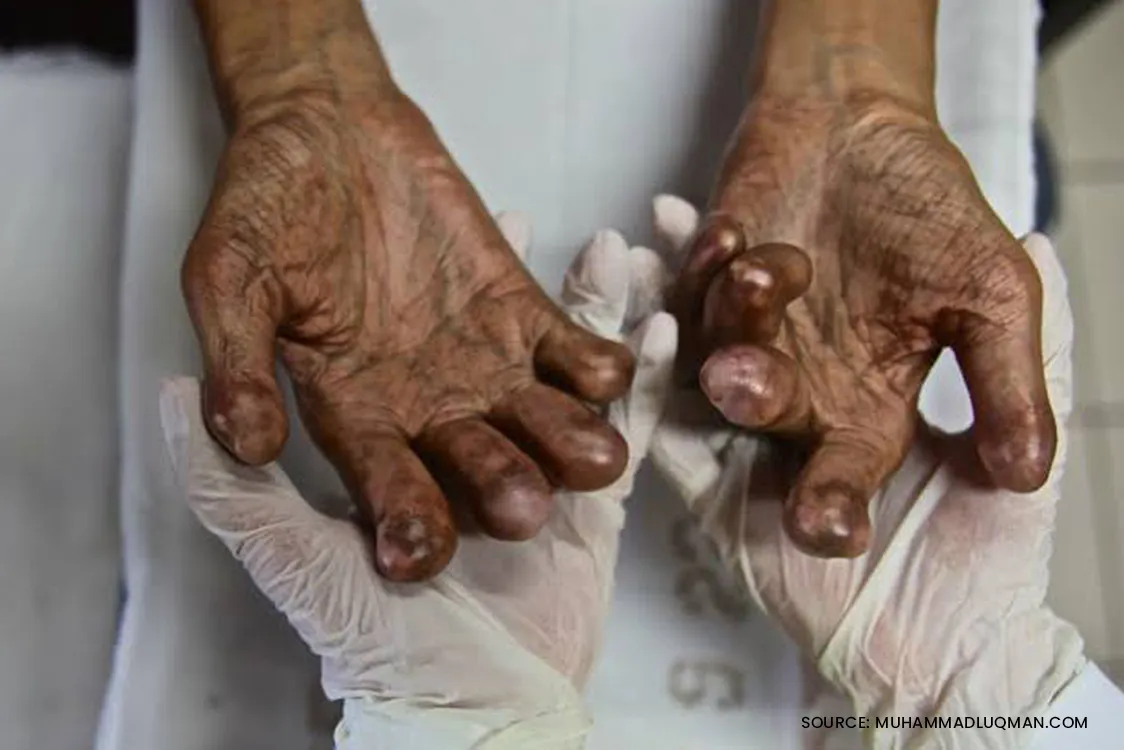
This condition can cause several other health complications, including organ damage, severe pain, and a reduced lifespan. Sickle cell anaemia symptoms typically start when babies are 5 to 6 months old. It not only causes anaemia but also causes immense pain, reduces growth, and affects many organs like lungs, heart, kidney, eyes, bones and the brain.
Here are three ways by which sickle cell disease can be reduced at a macro level.
Early Detection:
Timely detection of Sickle cell anaemia is important as it can help treat the patient before the case becomes severe. Early diagnosis enables the implementation of preventive measures, effective management strategies, and the development of personalized treatment plans as per the patient’s health specifications.
Neonatal screening for early diagnosis, penicillin prophylaxis, and immunization to control the infectious risk, have dramatically decreased Sickle cell disease (SCD) in other countries, where more than 90 percent of children had SCD. And withsuch preventive measures SCD diagnosed children have survived to adulthood*.
Prenatal Screening:
Prenatal screening involves testing couples who are planning to have a child. This screening is done to understand whether the parents have common genetic blood disorders like sickle cell anaemia and thalassaemia. If both partners are carriers of the sickle cell trait, there is a risk of passing the disease on to their children. Counselling can help couples understand their risks, explore various reproductive options, and make informed choices to reduce the likelihood of having a child with sickle cell anaemia. Sickle cell anaemia testing allows individuals and families to make informed decisions regarding family planning.
Testing can also help identify individuals at risk of having a child with the disease, enabling them to access appropriate prenatal care and interventions. Access to accurate and reliable prenatal diagnostic services is crucial in preventing children’s birth with sickle cell anaemia.
Newborn Screening:
Another effective method is newborn screening. In this screening, drops of blood from a heel prick are collected on a special type of paper. The haemoglobin from this blood is then tested in a lab. Early detection of SCD is extremely useful for improving the quality of life of a child with SCA or SCD. Therefore, neonatal screening for SCD is recommended. Newborn screening programs are essential in identifying infants with sickle cell disease at birth.
Early detection through newborn screening enables prompt medical intervention, including initiating preventive treatments, early management of complications, and follow-up care.
Early diagnosis and treatment have improved survival rates, reduced morbidity, and enhanced the overall well-being of children with sickle cell anaemia in other nations with high SCA cases.
Data Source: Sickle cell anaemia 11 times deadlier than thought, study finds | The Financial Express